What Are The Risks And Benefits Of C-Section Birth?
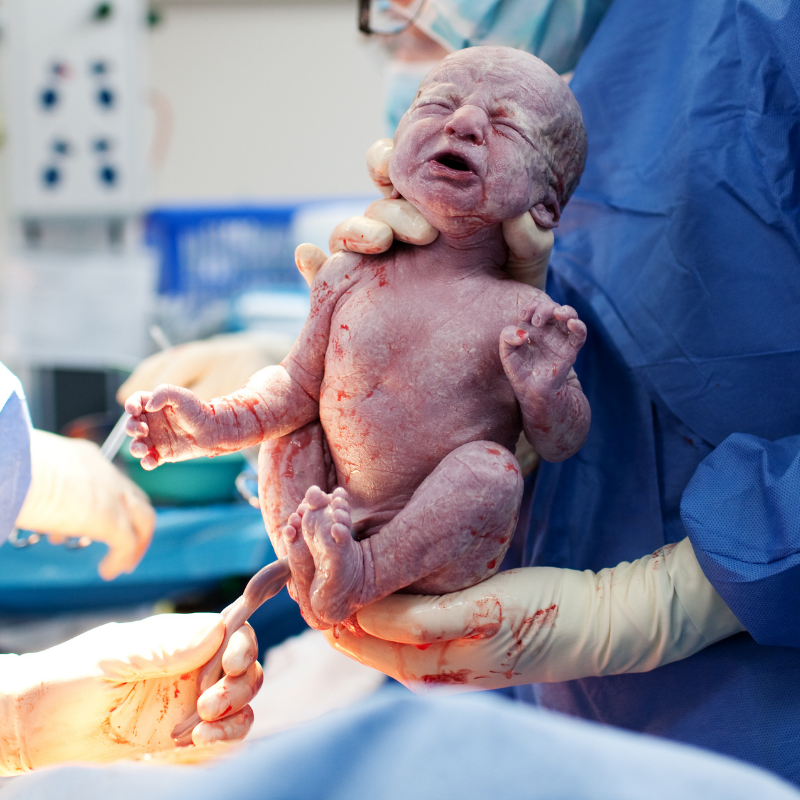
It’s important to know the risks and benefits of c-section birth.
Most expecting parents plan and hope to meet their baby after a normal and natural birth. Yet 1 in 3 babies in Australia are born via c-section.
Sometimes this is necessary for the safety of either mother and baby. C-sections can also happen as a result of the cascade of intervention. This means earlier interventions have disrupted the normal process of labour, leading to c-section being necessary to prevent further harm.
The World Health Organization recommend c-section should only be performed for medical reasons. Yet research is showing overuse of obstetric interventions is increasing with no evidence of medical need.
We cover this in our blog post Why Have A C-Section Birth?
Deciding to have a c-section isn’t something anyone should feel pressured into. You need to consider the risks and benefits of c-section birth for the short term. You also need to think about how a c-section birth might affect your future pregnancies and birth options.
To help you be as informed as possible about your birth options, in this blog we’re looking at the risks and benefits of c-section birth.
What are the benefits of a c-section?
The benefits of c-section centre around reducing the risk of harm to either mother or baby during labour and birth.
This means if normal labour and birth increases the chances either the mother or baby could be harmed or die, then the benefit of a c-section is to reduce that risk.
In rare situations, the fear of giving birth naturally is so extreme that it affects a woman’s mental health. This is known as tokophobia and can lead to pregnancy termination, avoiding prenatal care, and post traumatic stress disorder or other mental health disorders. After birth, it can affect a mother’s ability to bond with her baby. Planning a c-section in this situation may be of benefit.
There is some reduction in the risk of pelvic prolapse compared to vaginal birth, but this is controversial as it’s suggested this only benefits women who have already had surgery to correct prolapse.
Babies who have certain abnormalities or known health conditions which may require immediate life saving treatment may benefit from being born quickly at a certain point in pregnancy.
Risks of having a c-section
Risks of c-sections relate mostly around those that aren’t medically necessary. As we know, many women end up having a c-section as a result of interference with the natural process of labour.
Some will choose to have a c-section for no medical reason other than convenience but this is becoming rarer as health organisations are beginning to acknowledge the burden of c-section on the health system, women and babies.
C-section risks for mothers:
- A reaction to the anaesthetic used during the surgery can cause severe headaches.
- Needing to stay in hospital longer after birth
- Longer recovery period needed
- Blood loss that leads to needing a blood transfusion
- Risk of surgical injury to other organs
- Needing to have a hysterectomy during or after surgery
- Blood clots on the lungs or pelvic organs
- Infection of the bladder, uterus or the site of the incision, causing pain and discomfort in the short term, and lead to long term use of antibiotics and potentially further surgery
- Problems in future pregnancies, related to placenta position, scar rupture, or ectopic pregnancy forming in the uterine scar
- Scar tissue causing adhesions that lead to organs sticking to the abdominal wall or each other, causing pain and future health issues
Maternal death is increased after a c-section, compared to vaginal birth (4 times more likely after an emergency and 3 times more likely after planned c-sections.
C-section risks for babies
- There is a small risk of your baby being cut as the incision is being made. This is more likely to happen if your waters have broken before the surgery, you’re in active labour, the surgeon isn’t experienced, you’ve had a previous uterine incision
- Your baby is born prematurely, especially if you have chosen an elective or planned c-section. Estimated due dates are simply guesses of when your baby will reach full term and be ready for life outside the womb
- Breathing problems that require special care after birth. This can either be due to being born early, or the c-section was planned and labour hadn’t started. Contractions push fluid from your baby’s lungs ready for breathing. An elective c-section bypasses this process and causes fast, laboured breathing.
- Persistent pulmonary hypertension, which is when your newborn’s system doesn’t transition and continues to flow as it did in the uterus, increasing the blood pressure and lowering oxygen levels. This is more likely to occur in babies born by planned c-section
- Future health seems to be affected, with babies born via c-section being more likely to develop Type 1 diabetes, obesity, and asthma. It’s thought this is due to babies not being exposed to healthy bacteria in the birth canal
Babies born via c-section are more likely to be separated from their mothers for the first minutes to hours. This is the time when babies undergo the transition from womb to world and they’re innately hardwired to be close to their mother’s body to get all the benefits. Separation after c-section can impact early bonding and breastfeeding.
Being prepared for birth means being informed and considering all your options. Nurtured Birth offers a range of services to help you navigate whatever your birth journey ends up being.
Contact us to find out more about our birth education classes, workshops on choosing care providers, and birth doula services.






